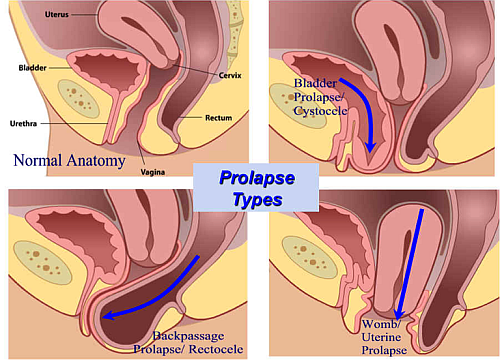
Pelvic Organ Prolapse
Prolapse" refers to a descending or drooping of organs. Pelvic organ prolapse refers to the prolapse or drooping of any of the pelvic floor organs, including:
Bladder
Uterus
Vagina
Small bowel
Rectum
Causes Pelvic Organ Prolapse
Anything that puts increased pressure in the abdomen can lead to pelvic organ prolapse. Common causes include:
Pregnancy, labor, and childbirth (the most common causes)
Obesity
Respiratory problems with a chronic, long-term cough
Constipation
Pelvic organ cancers
Surgical removal of the uterus (hysterectomy)
Genetics may also play a role in pelvic organ prolapse. Connective tissues may be weaker in some women, perhaps placing them more at risk.
Symptoms of Pelvic Organ Prolapse
Some women notice nothing at all, but others report these symptoms with pelvic organ prolapse:
A feeling of pressure or fullness in the pelvic area
A backache low in the back
Painful intercourse
A feeling that something is falling out of the vagina
Urinary problems such as leaking of urine or a chronic urge to urinate
Constipation
Spotting or bleeding from the vagina
Symptoms depend somewhat on which organ is drooping. If the bladder prolapses, urine leakage may occur. If it's the rectum, constipation and uncomfortable intercourse often occur. A backache as well as uncomfortable intercourse often accompanies small intestine prolapse. Uterine prolapse is also accompanied by backache and uncomfortable intercourse.
Treatment Options
If your physician determines that you are dealing with mild pelvic organ prolapse-asymptomatic—there is a good chance it can improve on its own. Watchful waiting is often the course of action, though it is not possible to identify whose POP will improve with time.
MANAGEMENT
Although there are limited non-surgical management options for POP, pessaries are often employed. Made of silicone, pessaries are devices that provide structural support when placed in the vagina. Since women come in all shapes and sizes, pessaries need to be fitted to the specific shape of the individual.
A successful pessary is one that is comfortable, is retained with Valsalva, and treats POP symptoms adequately. Pessaries do require upkeep and need to be removed and cleaned on a regular basis.
It is not unusual for local vaginal estrogen to be prescribed for use in conjunction with a pessary for comfort, lubrication, and to lower incidence of urinary tract infections.
In addition, there are many useful products that you might find useful in managing your condition.
BEHAVIORAL MODIFICATIONS
Many women find relief from Pelvic Organ Prolapse symptoms by performing targeted exercises. Typically, a physical therapist trained in this area can help create a customized plan that includes finding and strengthening the pelvic floor muscles.
Pelvic Floor Muscle Exercises
Biofeedback
Pelvic Floor Stimulation
SURGICAL TREATMENT
While reconstructive surgery for POP is an option, it must be noted that there is a 30% recurrence rate for women choosing this route. Prolapse repairs can be done transvaginally, abdominally, laparoscopically, and/or robotically (when a scope is placed through the belly button). Ultimately, the purpose of the surgery is to correct the anatomy as well as provide better bowel, bladder, and vaginal function.
Cystocele Repair - This surgery repairs a prolapsed bladder or urethra (urethrocele)
Hysterectomy - This is a complete removal of the uterus.
Rectocele Repair - A rectocele repairs the fallen rectum and small bowel (enterocele).
Vaginal Vault Suspension - Most commonly a laparoscopic procedure to repair the vaginal wall
Vaginal Obliteration - Closure of the vagina
While abdominal repairs are believed to have higher success rates, the increase in morbidity makes this also one of the riskier options. Less than optimal success rates has inspired physicians to look elsewhere. Vaginal grafts (made of synthetic and biologic materials) are being explored as a long-term solution to POP. Research is currently being conducted to determine if the benefits of using mesh grafts in POP surgical repairs for greater durability sufficiently outweighs the risks of undesirable adverse consequences.